Business and Digital Transformations for a Hospital to Improve Patient Engagement – A Case Study
As the healthcare industry moves to a more value-focused approach, hospital and healthcare organisations are being challenged to improve healthcare quality while also becoming more efficient in their service outcomes. Ehealth and its technological advances are providing hospitals the solutions and means to navigating healthcare’s shifting landscape. However, prior to the hospital integrating a new technology, it is important for them to first define the problem in relation to the service provision issue they are trying to solve.
Here we highlight the case study of a hospital who was challenged by year-on-year reduction in patient enrolments as well as poor retention in follow-up visits by patients. The hospital CEO cited a steady upward trend in payments for health insurance premiums as well as considerable government cuts in subsidising hospital fees, which culminated in the hospital making a record loss in its annual financial reporting.
i3 Consult’s initial approach to the problem, was to tackle the drastic reduction in footfall of the patient numbers as a priority. To this end, we conducted teleconference interviews with hospital internal stakeholders to identify knowledge gaps and blind spots from current and historical service provision profiles. These interviews were one-on-one structured or semi-structured conversations. Extended interviewing of consensually selected healthcare payer industry experts with adapted questions were performed for refinement and reflection of the internal findings. Focus group meetings consisting of 5 team members each from a cross-section of the hospital’s value chain were conducted to brainstorm on the critical success factors that would bolster and procure a greater enrolment of patients. As a further refinement strategy, surveys of closed research instrument design tested the attitudes and perceptions of current healthcare service offerings and clearly defined future ones to a selected pool of hospital enrollees. The objective here was to confirm strategies for synchronizing the hospital’s value chain with the healthcare needs of the community.
From the existing turnover of 1200 enrollees paying on average $US45 per month per adult for health insurance, this established a breakeven point from which both full-scale value chain (figure 1) and cost reduction analyses were conducted to clearly identify the organisational and operational transformations necessary for maximizing the profit margin of the hospital’s accounts. Similar analyses were conducted on the 10% private patient segment and commensurate strategies proposed.
A full SWOT audit of the hospital’s operational, technological (e.g. e-medical records) and clinical systems were conducted and reported in the roadmap for a new business model proposal. As for the hospital’s annual financial reports, a profiling method using financial ratios, e.g. liquidity, acid test and capital gearing ratios as well as current asset turnover rates, identified what to harvest, hold, grow, turnaround or find niche within the hospital’s current healthcare service portfolio.
As an additional value add to the business plan report, a structured audit was conducted on the current operational system of the hospital from the point of patient-in to the point of patient-out and from perspective of clinical outcomes. This clinical operational audit identified the key elements of a Plan Do Check Act system ensuring that there is compliance with regulated best practice. Based on the above findings and from evaluation of our in-house “STP” – Segmentation, Targeting, Positioning tools, a promotional campaign road map was constructed to procure enhanced enrollment of patient numbers and find new patient segments.
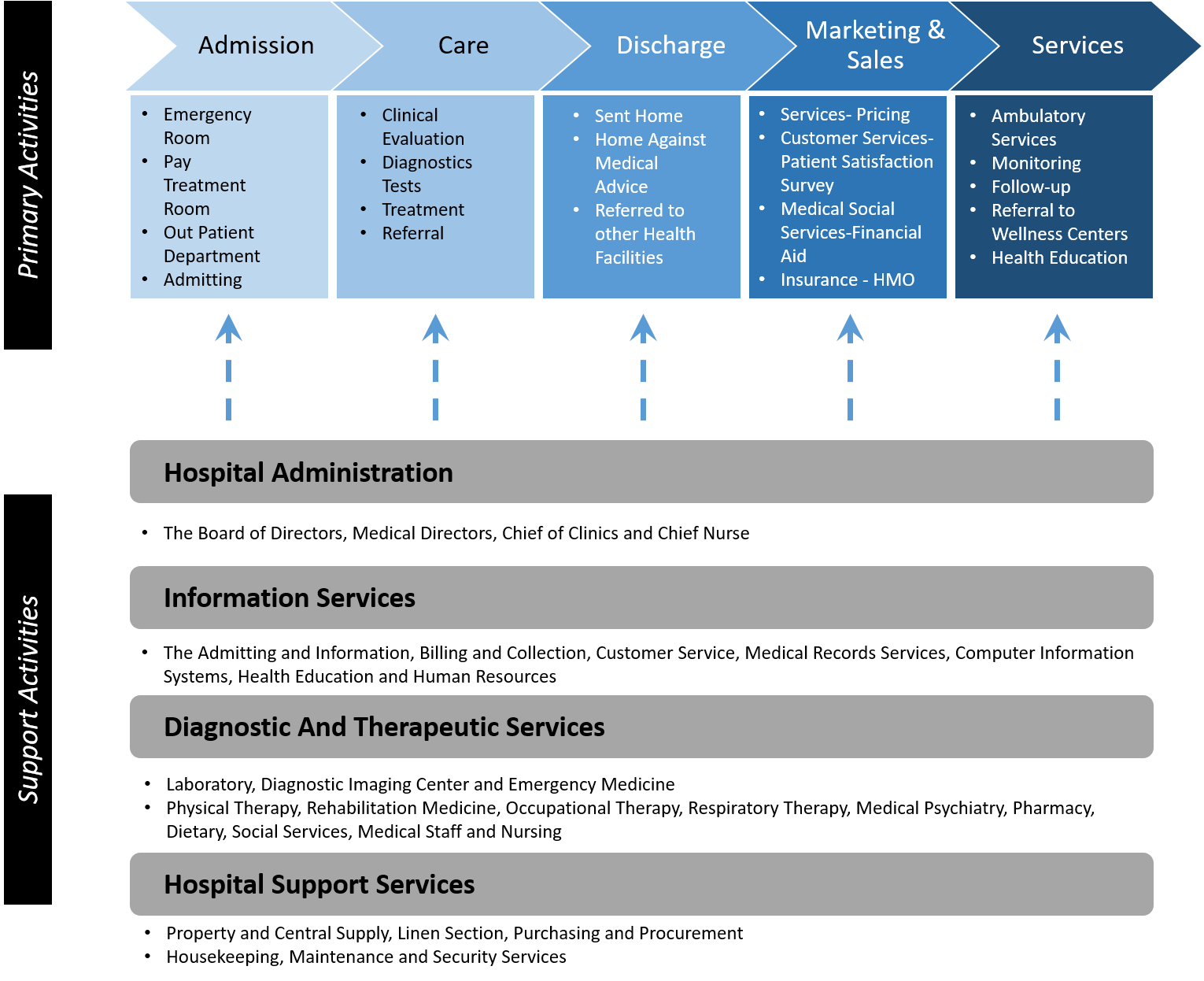
Source: Adopted to Michael E. Porter Value Chain model to the hospital. The Primary processes are activities devoted to care patients. The Support processes support primary activities by providing human, technical and material resources.
Figure 1: An Analysis of a Hospital Value Chain